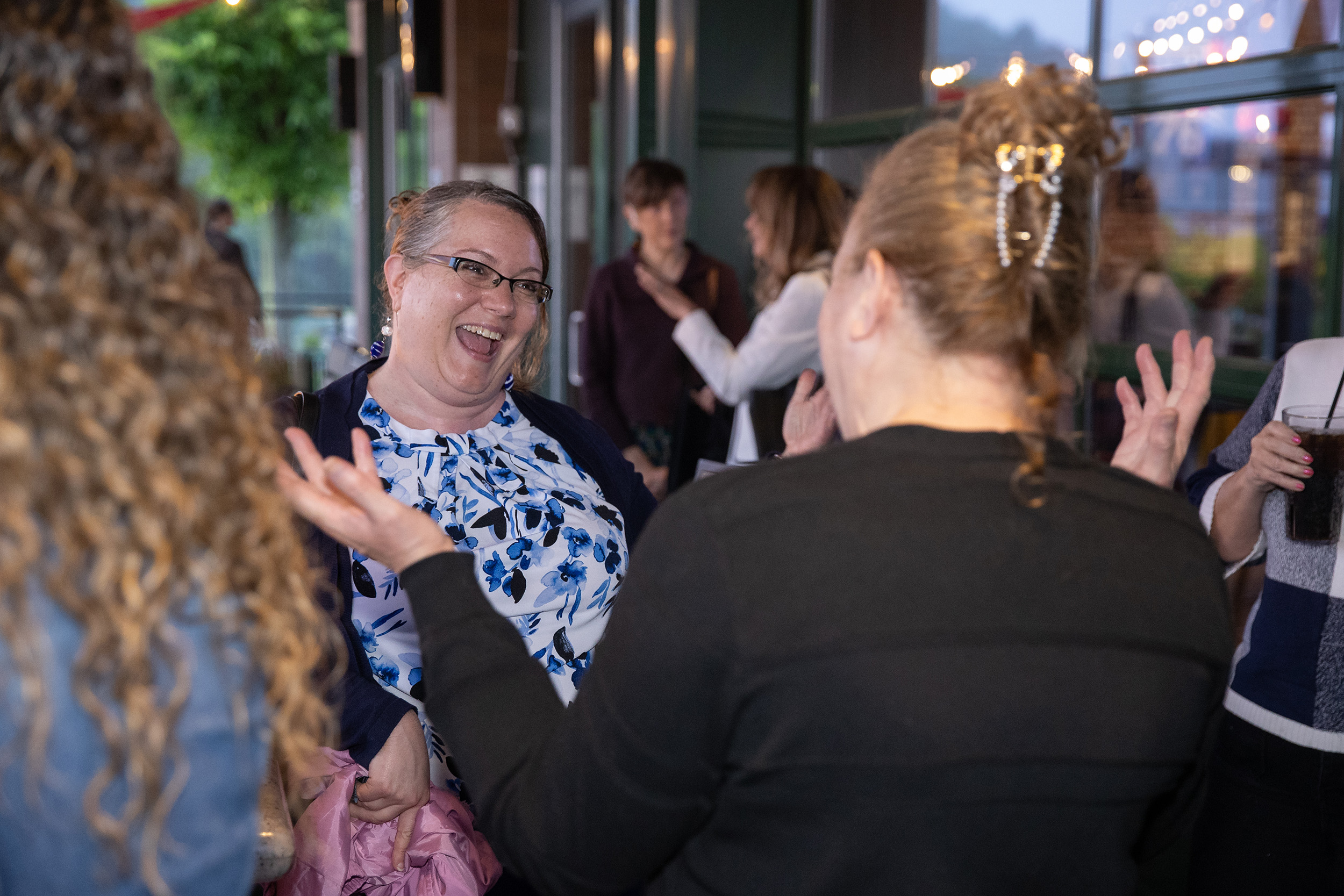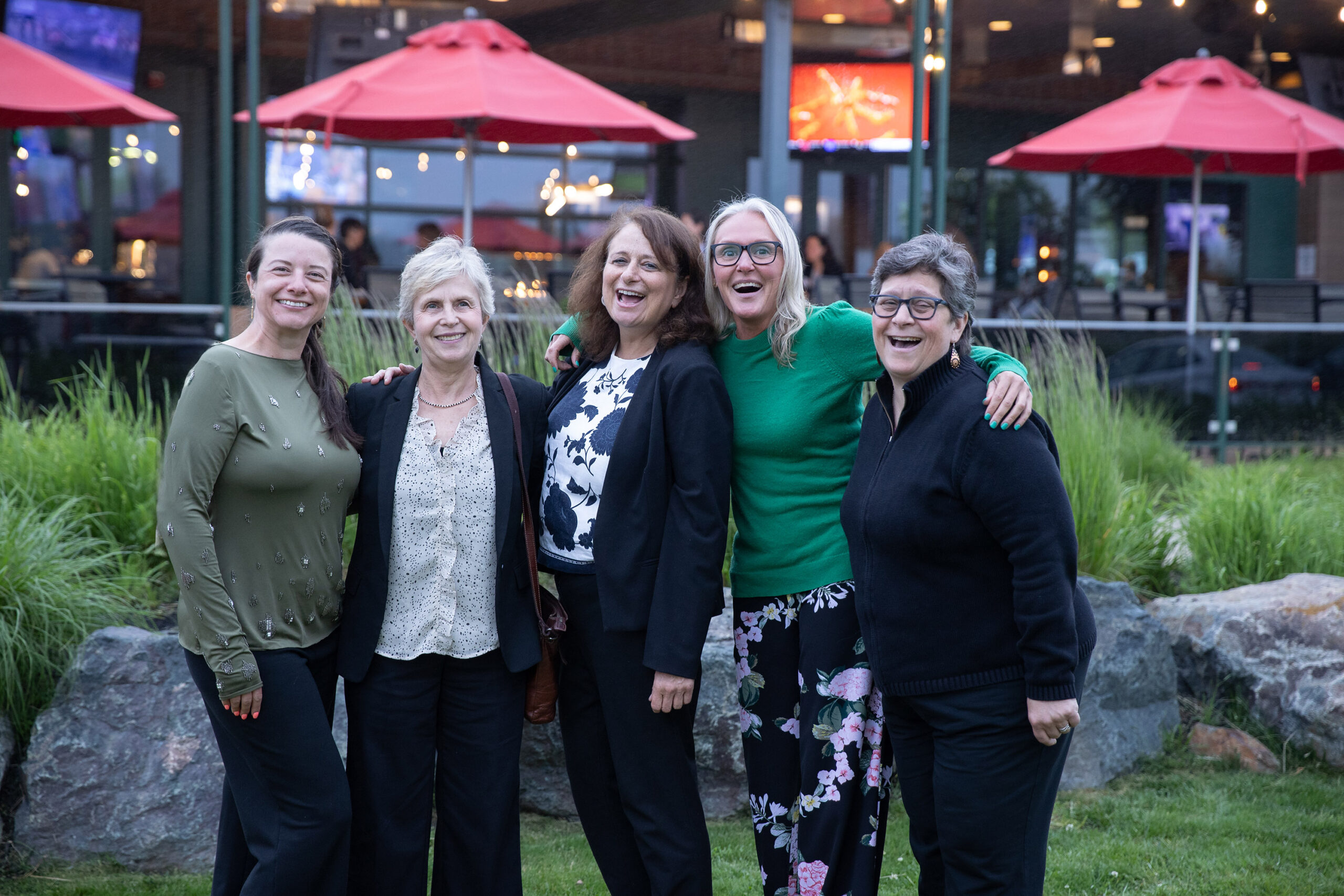AI in Healthcare: From Buzzword to Bedside Reality
Artificial intelligence (AI) has moved from a futuristic concept to a daily presence in healthcare, but what does that actually look like inside a hospital or clinical setting? At our WHCM Spring Forum, we hosted a panel featuring Colleen McGuire, Jeannette Curie, and Trish Rivard, where the conversation unpacked how AI is reshaping care delivery, operations, and the healthcare workforce—while also raising important questions about safety, equity, and trust. In a clinical environment, AI is a broad set of technologies that analyze data, recognize patterns, and support decision-making. Unlike traditional clinical decision support systems (CDS), which rely on fixed rules (“if X, then Y”), AI models learn from large datasets and continuously improve over time. This distinction matters. Traditional tools are static and predictable. AI is dynamic, adaptive, and can surface risks or insights clinicians might otherwise miss. What’s striking is how often AI is already embedded in workflows without clinicians even noticing. From radiology image prioritization to early sepsis alerts and automated documentation suggestions, AI is increasingly working in the background.
Healthcare has been slower in comparison to industries like finance and retail in adopting AI, but that gap is closing quickly. Several forces are driving this acceleration:
- Staffing shortages and burnout are pushing systems to find efficiency
- Financial pressures demand smarter resource utilization
- Advances in computing power and data availability have made AI more practical
- EHR integration capabilities are improving, making deployment easier
Today, AI’s most meaningful contributions are emerging in:
- Diagnostics and imaging: Faster, more accurate interpretation of scans
- Predictive analytics: Identifying patients at risk of deterioration or readmission
- Care pathways: Guiding evidence-based interventions in real time
Panelists emphasized that AI is not replacing clinicians—it’s augmenting them. The goal is better-informed decision-making, not automation of clinical judgment. In real-world settings, this translates to earlier interventions, fewer adverse events, and improved patient safety.
Adopting AI requires organizational readiness:
- High-quality, standardized data
- Seamless integration with the EHR
- Strong clinical engagement and trust
- Clear governance structures
Common barriers include fragmented data systems, cultural resistance, and unclear ROI. Many organizations struggle not with whether to invest in AI, but where to start.
When asked about the right place to start, panelists highlighted identifying a clear operational or clinical pain point to be solved, having measurable outcomes, and realizing what opportunity there is to scale across the organization.
Balancing innovation with patient privacy is critical. AI introduces new cybersecurity risks, including data exposure and model manipulation, requiring stronger governance and protections. One of the most pressing questions: Who is accountable when AI contributes to a clinical decision? The answer isn’t fully settled, but leading organizations are establishing governance frameworks that include multidisciplinary AI oversight committees, creation of clear policies on tool validation and use and defined accountability structures. AI governance is quickly becoming as essential as financial or clinical governance.
Over the next 3–5 years, AI is poised to further transform healthcare through more personalized treatment recommendations, real-time clinical decision support, advanced automation of administrative tasks and predictive, system-wide capacity management.
AI should be about redesigning systems to work better for both patients and providers. The organizations that succeed will be those that balance innovation with responsibility, invest in the right foundations, and keep patients at the center of every solution.